OCD vs. Autism: Similarities and Differences
Unveiling the similarities and differences between OCD and Autism, helping you understand their core features and treatment approaches.

Understanding OCD and Autism
To comprehend the similarities and differences between OCD (Obsessive-Compulsive Disorder) and Autism, it's essential to have a clear understanding of each condition individually.

What is OCD?
OCD is a mental health disorder characterized by recurring and intrusive thoughts (obsessions) that lead to repetitive behaviors (compulsions). People with OCD often experience intense anxiety and distress, which they try to alleviate through these compulsive behaviors. Common obsessions include concerns about cleanliness, order, or safety, while compulsions may involve excessive handwashing, checking, or arranging objects.
It's important to note that OCD is not simply a preference for organization or cleanliness. It is a clinically diagnosed condition that significantly impacts an individual's daily life and functioning.
What is Autism?
Autism, or Autism Spectrum Disorder (ASD), is a developmental disorder that affects communication, social interaction, and behavior. Individuals with autism may have difficulties with social skills, repetitive behaviors, and sensory sensitivities. Autism is a spectrum disorder, meaning it encompasses a wide range of symptoms and severity levels, from mild to severe.
While the exact causes of autism are not fully understood, it is believed to involve a combination of genetic and environmental factors. Autism is typically diagnosed in early childhood, as symptoms become apparent during early developmental milestones.
Understanding the distinct characteristics of OCD and autism is essential in recognizing the similarities and differences between the two conditions. By delving deeper into these aspects, we can gain a better understanding of how OCD and autism manifest and how they can be differentiated.
Exploring Similarities
When examining the relationship between Obsessive-Compulsive Disorder (OCD) and Autism Spectrum Disorder (ASD), it is important to recognize that these are distinct conditions with their own unique features. However, there are also notable similarities between OCD and Autism that can help shed light on their shared characteristics.
Overlapping Symptoms
OCD and Autism share some common symptoms, although they may manifest differently in each condition. Here are some of the overlapping symptoms between OCD and Autism:

Shared Challenges
Individuals with OCD and Autism face similar challenges in their daily lives. These challenges can impact various aspects of functioning, including social interactions, daily routines, and emotional well-being. Here are some shared challenges experienced by individuals with OCD and Autism:
- Social Difficulties: Both conditions can lead to social challenges. Individuals with OCD may struggle with social interactions due to anxiety or fear of contamination, while individuals with Autism may experience difficulty understanding social cues or engaging in reciprocal communication.
- Impact on Daily Life: OCD and Autism can significantly impact daily routines and functioning. The need to perform rituals or repetitive behaviors in OCD can consume a substantial amount of time, affecting productivity and quality of life. Similarly, individuals with Autism may face challenges in adapting to changes in routines or may require additional support to navigate daily tasks.
- Emotional Distress: Both conditions can cause emotional distress. Individuals with OCD may experience high levels of anxiety, fear, or guilt related to their obsessions and compulsions. Similarly, individuals with Autism may struggle with emotional regulation and may experience heightened levels of anxiety, frustration, or sensory overload.
- Co-Occurrence: It is not uncommon for individuals to have both OCD and Autism. Research suggests a higher likelihood of co-occurrence between these conditions compared to the general population. When OCD and Autism coexist, it can present additional challenges and complexities in diagnosis and treatment.
By recognizing the overlapping symptoms and shared challenges between OCD and Autism, we can enhance our understanding of these conditions and provide better support and resources for individuals affected by them.
Recognizing Differences
While OCD and autism share some similarities in terms of overlapping symptoms and challenges, it is important to recognize the core features that distinguish these two conditions.
Core Features of OCD
Obsessive-Compulsive Disorder (OCD) is characterized by the presence of obsessions and/or compulsions that cause significant distress and interfere with daily functioning. The core features of OCD include:
- Obsessions: Intrusive and unwanted thoughts, images, or urges that repeatedly occur in an individual's mind. These obsessions are often distressing and can lead to anxiety.
- Compulsions: Repetitive behaviors or mental acts performed in response to obsessions, usually with the aim of reducing anxiety or preventing a feared outcome. Compulsions are not connected to the actual event but are driven by the individual's belief that they can prevent harm or alleviate distress.
- Awareness of irrationality: Individuals with OCD are typically aware that their obsessions and compulsions are irrational or excessive, but they feel compelled to engage in these behaviors to manage their anxiety.
Core Features of Autism
Autism, or Autism Spectrum Disorder (ASD), is a neurodevelopmental disorder that affects social interaction, communication, and behavior. The core features of autism include:
- Social communication challenges: Difficulty with social interactions and communication, including nonverbal cues, maintaining eye contact, and understanding social norms.
- Restricted and repetitive behaviors: Engaging in repetitive behaviors or having specific interests or fixations. These behaviors can include repetitive movements, adherence to routines, and resistance to change.
- Sensory sensitivities: Heightened or reduced sensitivity to sensory input, such as sound, light, touch, or taste. Individuals with autism may experience sensory overload or seek sensory stimulation.
- Difficulties with social relationships: Difficulty forming and maintaining relationships, understanding social cues, and developing empathy.
- Cognitive strengths and challenges: Variability in cognitive abilities, with some individuals displaying exceptional skills in specific areas, such as math or music, while others may have intellectual disabilities.
It's important to note that while some individuals may have both OCD and autism, these conditions are distinct and can coexist independently.
Understanding the core features of OCD and autism helps in recognizing the differences between these two conditions. This knowledge is crucial for accurate diagnosis and appropriate treatment approaches tailored to the specific needs of individuals with either OCD or autism.
Diagnosis and Assessment
When it comes to diagnosing and assessing Obsessive-Compulsive Disorder (OCD) and Autism, there are specific criteria that healthcare professionals use to identify these conditions. Understanding the diagnostic criteria for each can help differentiate between the two.
Diagnostic Criteria for OCD
To diagnose OCD, healthcare professionals refer to the Diagnostic and Statistical Manual of Mental Disorders (DSM-5) published by the American Psychiatric Association. The DSM-5 outlines the following criteria for an OCD diagnosis:
- Presence of obsessions, compulsions, or both:
- Obsessions: Recurrent and persistent thoughts, urges, or images that are intrusive and cause distress.
- Compulsions: Repetitive behaviors or mental acts that an individual feels compelled to perform in response to obsessions or according to rigid rules.
- The obsessions or compulsions are time-consuming (take more than one hour per day) or cause significant distress or impairment in daily functioning.
- The symptoms are not better explained by the presence of another mental disorder.
Diagnostic Criteria for Autism
The diagnosis of Autism Spectrum Disorder (ASD) is also based on the criteria outlined in the DSM-5. The diagnostic criteria for Autism include:
- Persistent deficits in social communication and social interaction across multiple contexts:
- Social-emotional reciprocity difficulties.
- Nonverbal communication deficits.
- Challenges in developing, maintaining, and understanding relationships.
- Restricted, repetitive patterns of behavior, interests, or activities, as manifested by at least two of the following:
- Stereotyped or repetitive motor movements, use of objects, or speech.
- Insistence on sameness, inflexible adherence to routines, or ritualized patterns of behavior.
- Highly restricted, fixated interests that are abnormal in intensity or focus.
- Hyper- or hypo-reactivity to sensory input or unusual interest in sensory aspects of the environment.
- Symptoms must be present in the early developmental period.
- Symptoms cause clinically significant impairment in social, occupational, or other important areas of functioning.
It's important to note that a comprehensive evaluation by a qualified healthcare professional is necessary to make an accurate diagnosis of OCD or Autism. The diagnostic process involves a thorough assessment of an individual's symptoms, developmental history, and behaviors.
By understanding the specific diagnostic criteria for OCD and Autism, healthcare professionals can differentiate between these conditions and provide appropriate support and treatment tailored to each individual's needs.
Treatment Approaches
When it comes to treating OCD and autism, different strategies are employed to address the unique challenges associated with each condition. While there are some overlapping therapeutic techniques, it's important to tailor the treatment approach to the specific needs of individuals with OCD or autism.
OCD Treatment Strategies
OCD treatment typically involves a combination of psychotherapy, medication, and self-help strategies. The primary psychotherapy approach used for OCD is Cognitive Behavioral Therapy (CBT), specifically a subtype known as Exposure and Response Prevention (ERP). ERP involves gradually exposing individuals to their obsessions and preventing the accompanying compulsive behaviors, thereby helping them develop healthier coping mechanisms.
In addition to therapy, certain medications can be prescribed to manage OCD symptoms. Selective Serotonin Reuptake Inhibitors (SSRIs) are commonly used as they help regulate serotonin levels in the brain, which can alleviate anxiety and obsessions. Antidepressants and antipsychotics may also be prescribed in some cases.
Self-help strategies, such as practicing mindfulness and stress reduction techniques, can complement formal treatment. Support groups and online resources provide a platform for individuals with OCD to share their experiences and learn from others in similar situations.
Autism Treatment Strategies
The treatment of autism focuses on improving communication skills, social interactions, and managing behavioral challenges. Applied Behavior Analysis (ABA) is a widely used therapy for individuals with autism. ABA involves breaking down behaviors into smaller components and using positive reinforcement to encourage desired behaviors.
Speech therapy is often employed to enhance communication skills, while occupational therapy helps individuals develop daily living skills and address sensory sensitivities. Social skills training is another important aspect of autism treatment, where individuals learn appropriate social cues and behaviors through structured sessions.
Medications may also be prescribed to manage specific symptoms associated with autism, such as hyperactivity, aggression, or anxiety. However, it's important to note that medication is not a primary treatment for autism and is typically used in conjunction with other therapeutic interventions.
Table: Medications Used in OCD and Autism Treatment
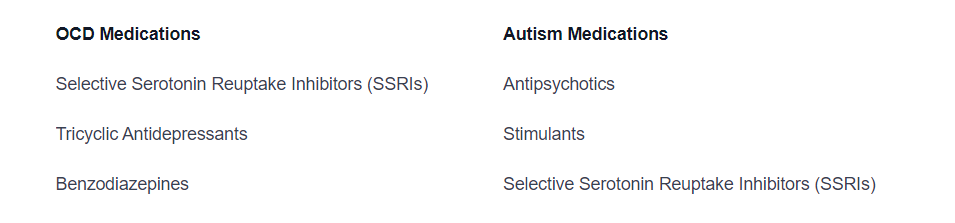

By employing these treatment strategies, individuals with OCD or autism can improve their quality of life and manage their symptoms effectively. It's important to remember that treatment plans should be personalized to address the unique needs and challenges of each individual, and involve a multidisciplinary approach that considers their specific circumstances.
Living with OCD or Autism
Living with OCD or autism can present unique challenges for individuals and their families. However, there are coping strategies, support systems, and resources available to help navigate these conditions and improve quality of life.
Coping Strategies
Coping strategies play a significant role in managing the symptoms and daily challenges associated with OCD or autism. These strategies may vary depending on the individual and their specific needs. Here are some commonly used coping strategies:
- Establishing routines: Creating structured daily routines can provide a sense of predictability and stability, which can be particularly helpful for individuals with autism.
- Setting realistic goals: Breaking down tasks into manageable steps and setting realistic goals can reduce stress and increase a sense of accomplishment.
- Practicing relaxation techniques: Techniques such as deep breathing, meditation, and mindfulness exercises can help reduce anxiety and promote emotional well-being.
- Engaging in hobbies and interests: Pursuing hobbies and interests can serve as a positive distraction and provide a source of enjoyment and fulfillment.
- Seeking support: Connecting with support groups, therapy, or counseling can offer a safe space to share experiences and learn from others facing similar challenges.
Support Systems and Resources
Having a strong support system is crucial for individuals living with OCD or autism. This support can come from various sources, including:
- Family and friends: Loved ones can provide emotional support, understanding, and encouragement in navigating the complexities of OCD or autism.
- Educational and occupational support: Schools and workplaces can offer accommodations, specialized programs, and support services to help individuals succeed in academic and professional settings.
- Mental health professionals: Psychiatrists, psychologists, and therapists with expertise in OCD or autism can provide guidance, therapy, and treatment options tailored to individual needs.
- Support organizations: Numerous organizations offer resources, educational materials, and online communities to connect individuals and families affected by OCD or autism. These organizations can provide valuable information and support networks.
- Government and community services: Local government agencies and community organizations may offer assistance programs, financial support, and access to specialized services.
It's important for individuals and their families to explore and utilize these support systems and resources to ensure comprehensive care and a higher quality of life.
Living with OCD or autism can be challenging, but with the right coping strategies and support systems in place, individuals can effectively manage their symptoms, enhance their well-being, and thrive in their daily lives.
Sources
https://www.abtaba.com/blog/ocd-vs-autism
https://www.medicalnewstoday.com/articles/ocd-vs-autism
https://www.embarkbh.com/blog/ocd/ocd-and-autism/
Similar articles
We’re here to help you

Our team is here to assist you in this process. Contact us for any assistance.
it’s easy to apply
We Accept Most Insurances
Our in-network insurance partnerships make ABA therapy more accessible to families throughout our service areas.







Our Insurance Process
We'll request your insurance details to help us verify your plan's coverage for ABA therapy. Once we've received this information, we'll walk you through your benefits, including copayments, deductibles and out-of-pocket maximums, so you know what to expect in advance.
Our team will then handle the preauthorization and all the necessary paperwork.
.svg)




















.jpeg)


































.jpeg)




.jpeg)






.jpeg)










.jpeg)